Experts fear surge in infectious diseases amid Afghan refugee influx
Leishmaniasis was earlier mostly reported in bordering areas of Pakistan and Afghanistan
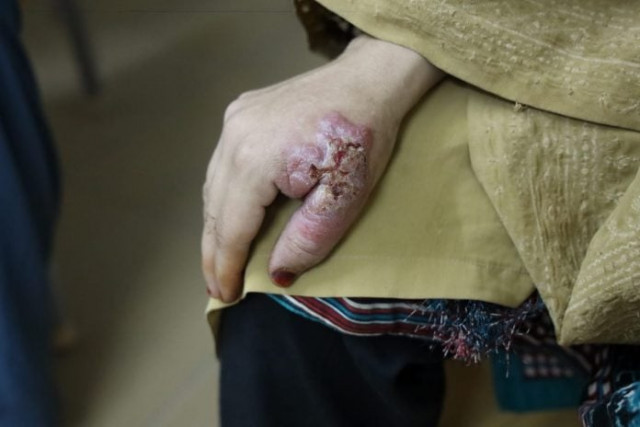
Hanzala Hamzullah, a middle-aged businessman with bulky appearance, considered an itching skin rash on toes of his right foot as a routine reaction to a mosquito bite, but extra swelling, severe pain and conversion of infected site into a fully blown-up septic lesion, made him concerned about the affliction.
“Initially, I did self-medication by applying different skin ointments for the treatment of the lesion, but the infection keeps on aggravating forcing me to consult a specialist dermatologist,” recalls Hanzala while speaking to APP at his shop in Peepal Mandi, city’s busiest market named after the oldest Banyan tree that was revered in past for its mythological connection with Lord Buddha.
Laboratory tests diagnosed the cause of the painful lesion as the Cutaneous Leishmaniasis (CL) infection, a parasitic skin disease transmitted through the bite of sand fly. With face expression clearly reflecting pain, he is enduring while removing blood-stained gauze to uncover coin-size skin ulcer. Hanzala complained that the infection started on August 5, 2021, and to date he has not recovered from this extremely agonising illness, disallowing him to walk and even sleep properly.
Like Hanzala, thousands of victims pass through the same critical phase of pain, severe stigma and psychological trauma due to this infectious disease, which is registering a surge in the northwestern region of the country near bordering areas with Afghanistan.
Read: UNHCR to help promote refugees’ handicrafts in Balochistan
Zakia, 25, from Peshawar’s peripheries, was also found concerned about the permanent scare she has been faced with due to a five months delay in the treatment of the infection because of her pregnancy. Holding a newborn infant in her lap at the Naseerullah Khan Memorial Hospital in Peshawar, the only specialised treatment centre for CL, Zakia told the news agency that she has shifted to her sister’s home located in the vicinity of the hospital to get a proper treatment to avoid lifelong disfigurement.
“Zakia got infected twice, at hand and ankle, in the fourth month of her pregnancy and have to wait till delivery to start taking meglumine antimoniate, first-line treatment for CL, as it is not suitable for pregnant women and people with cardiac issues,” informed Faqeer Hussain, supervisor of the Leishmaniasis treatment centre.
“Treatment for Zakia will continue for 28 days, but the lesions are likely to leave big scars, probably cause a physical disfigurement, for which she would require to see a plastic surgeon,” whispered Hussain to avoid the patient from hearing of his assessment. “Cutaneous Leishmaniasis is a skin disease ranging from self-healing lesions to large skin ulcers and is caused by a protozoan parasite of genus Leishmania transmitted through sand-fly,” apprises Dr Akram Shah, a PhD scholar on Parasitology.
Based on the epidemiology of the disease, it is divided into two forms, cutaneous leishmaniasis, which is both zoonotic including animal reservoir host in transmission and anthroponotic which is solely transmitted through infected humans. While the second and dangerous form is Visceral Leishmaniasis, which is fatal but fortunately not widespread in the region, explains Dr Akram.
He said that Leishmaniasis was earlier reported mostly in the bordering areas of Pakistan and Afghanistan within proximity of refugees’ settlements. However, now it has become endemic in this country due to mass movement and frequent border crossing, expanding infection range to other localities. In case of refugees influx due to changing political dynamics in Afghanistan, an impetus can be caused to the already existing infectious diseases and raise public health concerns in Pakistan, he added.
Experts believe that and increase in the movement of people, climatic change, urbanisation and deforestation are causing the spread and a surge in zoonotic and vector-borne diseases like CL, dengue, malaria, chikungunya, Congo, etc.
To substantiate this claim, they give the example of the dengue infection that has now become a regular epidemic since 1994 when it was first reported, in three provinces of the country, barring Balochistan.
“Pakistan is hosting 1.4 million registered Afghan refugees for the last four decades while an additional number of 850,000 of the Afghan nationals are staying here as Afghan Citizens,” informed Qaiser Khan Afridi, spokesman of the UNHCR. “If restrictions lifted and refugees are allowed to cross the border, a large influx is expected to arrive here due to economic hardship and harsh winter,” he added.
Read More: Decision on Indian wheat to Afghanistan expected soon
Considered as the `Poor’s affliction’ because of its occurrence in the rural and mostly slum dwellings, CL remained neglected by health teams until 2018 when an outbreak of the disease caused a largescale infection brought it into the limelight. In 2018 around 28,000 people were infected from CL in the tribal region and adjacent southern districts of Khyber-Pakhtunkhwa.
The outbreak gave way to the adoption of preventive measures, which helped in containing the disease and the cases of the infection in K-P gradually dropped to 24,131 in 2019, 18,652 in 2020, and 11,390 in the first 10 months of 2021. In Balochistan, the cases were contained from 18,495 in 2019 to 13,457 in 2020. While in the current year a total of 9,978 cases were registered till October 2021 in the province.
According to the WHO’s Country Profile for Leishmaniasis, Pakistan has registered about 16,648 cases in 2015. While at the global level, around 700,000 to one million cases occur annually. "The Medicines Sans Frontier (MSF), an international medical humanitarian association that came for the help of patients after the outbreak of CL in 2018, treated around 4,946 patients in 2020 at its three centers established in Peshawar, Bannu and Quetta cities,” says Zahra Shoukat, the communication officer at the MSF Pakistan. “[The] MSF is offering free-of-cost services to patients from southern districts of K-P and Balochistan where the disease is endemic,” Zahra added.
“In Pakistan, both Visceral and Cutaneous Leishmaniasis are prevalent but the high burden of CL is found in the southwestern province of Balochistan and K-P, located along the 2,600-kilometer-long porous border with Afghanistan,” reveals a study titled `Systematic Review of Leishmaniasis in Pakistan’, published in the Journal of Parasitology on August 6, 2021.
“Leishmaniasis is widening its horizon from endemic to non-endemic sites due to rapid urbanisation, deforestation and a large scale dispersion of the human population,” mentions Dr Nazma Habib Khan, a PhD on Leishmania Diagnostics from the London School of Hygiene and Tropical Medicine, who was also part of the three members’ team that conducted the above-stated study.
According to Dr Qaiser Khan, assistant professor at the Zoology Department of Peshawar University, Leishmaniasis became prevalent in the country after spreading from its pocketed ranges in the bordering region. “We have around 17 to 18 species of sand fly and when it bites an infected person, the transmission cycle starts jumping from one human to another.”
The disease needs to be given due consideration by conducting research on the breeding cycle of sand flies, vector biology, infection control measures, and drugs used in the treatment, as currently, they are around 70 years old, he suggested.
Read More: Health DG denies reports of new virus
He also recommended adopting the `One Health’ approach, involving multiple sectors to work together to achieve better public health outcomes, for finding out all the characteristics of the disease through the involvement of epidemiologists, entomologists, microbiologists and ecologists as well.
The burden of disease was increasing in Balochistan as it has been reported in 17 out of total 33 districts, stated Dr Khalid Qumbarani, programme manager of the Vector Control Programme Balochistan.
In an interview with APP, Dr Khalid said "our dependency was on the WHO in obtaining injections that provide 5,000 vials on a yearly basis, while we need 300,000 vials for treating 12,000 registered and unregistered patients."
The K-P government purchased 170,000 vials from the WHO for treatment of CL patients, who are getting treatment in 71 centers set up in the province, informed Dr Rehman Afridi, programme manager of the Integrated Vector Control Programme K-P.
“[The] WHO is providing injections for treatment of CL free-of-cost but in limited numbers due to its non-availability in the open market,” says Dr Muhammad Babar Alam, the head the WHO sub-office. He appreciated the decision taken by the K-P government of purchasing injection as per the increasing number of patients.
However, Dr Babar agreed that a refugee influx can raise the risk of an increase in infectious diseases because population density was the major source of the spillover of contagion.



















COMMENTS
Comments are moderated and generally will be posted if they are on-topic and not abusive.
For more information, please see our Comments FAQ