Growing concerns: About 10m Pakistanis are infected with hep C
Sindh has a prevalence rate of 5 per cent: PMRC.
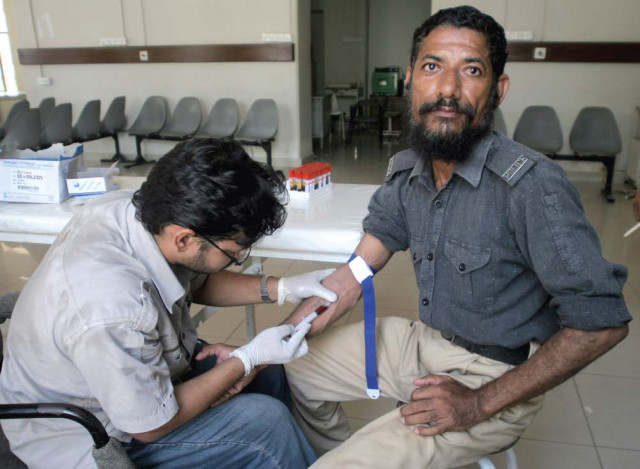
Practices such as the reuse of syringes and transfusing unscreened blood remain common in the majority of rural hospitals and even some urban centre hospitals.
There are an estimated 10 million people infected with hepatitis C in Pakistan; they make up almost six per cent of the population.
“This is a very, very high prevalence rate for any country,” said gastroenterologist and Pakistan Medical Research Council (PMRC) Executive Director Dr Huma Qureshi. “In my opinion the situation is already out of control and needs to be tackled very seriously.” Most countries worldwide barely breach the one to 1.2% prevalence mark. Pakistan is still better off than Egypt and Italy, however, whose prevalence rates go into double digits.
Hepatitis C is generally caused by a viral infection and leads to the inflammation of the liver. Symptoms include abdominal pain, dark-coloured urine, fatigue, itching and vomiting. Unlike with hepatitis B, there is no vaccine for hepatitis C and prevention is the only shield people have. The infection spreads through unsafe blood transfusions, contact with contaminated blood, unprotected intercourse and sharing personal hygiene items such as toothbrushes with an infected person.
“This [unethical medical practices] is not just true for rural areas,” said Qureshi. “Even at major hospitals, such as Jinnah Postgraduate Medical Centre, Abbasi Shaheed Hospital and Civil Hospital, Karachi, the reuse of syringes and contact with contaminated blood remains a grave cause for concern.”
The University of Karachi hosted a seminar on the topic on Saturday where Dr Aqueel Ahmed of the Department of Microbiology spoke on the topic. Over 70% of HCV infected patients become chronic and the infection may prove fatal. However, it is not all bad news, despite expensive treatment and fatality, early detection of hepatitis C, together with treatment, can help.
“Genotypes 3a and 3b, amongst 11 genotypes of hepatitis, are found to be the most common,” Ahmed said. “Patients with these genotypes also have good chances of response rate to therapy.” There are of course factors which make some people more prone to disease than others. This includes men, elderly people, and those co-infected with HIV or hepatitis B. Alcohol and too much iron in one’s system also make you too susceptible to infection. Making matters worse, 20 to 30% patients develop psychological disorders such as depression, Ahmed added.
Consultant gastroenterologist at the Sindh Institute of Urology and Transplantation Dr Zaigham Abbas explains the reason behind this sudden burst of hepatitis C infections in the population. “Many of these are due to case findings,” he explained. This means that people infected previously are being screened now and included in the data. “So while they are not really new cases this does not mean that it [hep C] is not spreading because it is.”
Screening was, and has, become a prerequisite for many procedures now - from people applying for immigration, visas, jobs and enrolment into the army to blood donations. In fact, experts say most are people are unaware that they have been infected till they test positive.
Published in The Express Tribune, November 28th, 2011.



















COMMENTS
Comments are moderated and generally will be posted if they are on-topic and not abusive.
For more information, please see our Comments FAQ