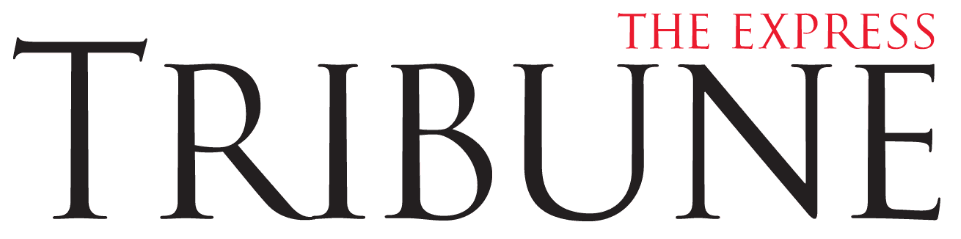For most of human history, losing weight was never a goal. Survival was. Across centuries of famine, food scarcity, and physically demanding lives, the human body evolved to store energy whenever it could. Fat was insurance against hunger, not something to be feared. In many cultures, including the subcontinent, a fuller body even signalled prosperity, fertility, and health.
Then came abundance. It changed our perceptions, practices and goals. The 20th century saw mass food production making calories cheap and plenty, while increasingly sedentary lifestyles became common. At the same time, thinness was elevated into a cultural ideal by fashion, film, advertising, and now social media. What was once a natural response to scarcity came to be seen as a personal failing, fuelling a billion-dollar dieting industry built on discipline, denial, and repeated cycles of hope and relapse.
A new era
But now, a new weight-loss chapter is unfolding. While fat liberationists are still working to de-stigmatise fatness and work towards a more equitable society for people of all body types, in quest of ideal thinness, the global weight management market is experiencing rapid growth, valued at approximately 150–160 billion US dollars in 2023–2024 and projected to exceed 300 billion dollars by 2030–2032. Growth is driven by rising obesity rates—affecting 2.5 billion adults in 2022—and the surge in demand for GLP-1 medications, which could create a 150 billion dollar market alone. The global anti-obesity market is projected to grow from approximately 160.15 billion dollars in 2024 to 328.24 billion dollars by 2032, reflecting a compound annual growth rate of 8.3% to 9.94%. This growth is being driven by the high prevalence of obesity—affecting 16% of adults worldwide in 2022—and the rapid rise of anti-obesity medications such as Ozempic and Zepbound.
But beneath the excitement lies a more complicated question. Is this truly a revolution in health — or simply the latest turn in a long history of trying to control the body? And perhaps the most pressing question of all is: who is this revolution really for? But first, let’s take a peek into weight-loss history.
The beginning
For centuries, dieting existed in Ancient Greece, but only as a holistic approach to physical and mental health. It wasn’t until the 19th century that the concept of dieting as primarily a way to lose weight or change one’s body first appeared.
The modern Western obsession with dieting and weight loss can be traced back to 1863, when William Banting, a man frustrated by his own struggle with weight began documenting his personal efforts to shed the extra weight — unconsciously launching one of the earliest diet trends in the Western world. At 64, he stood at 5’5” and weighed 202 pounds.
When he started to lose his hearing, Banting turned to surgeon William Harvey who, researching how sugar, fats, and starches influenced the body, recommended that Banting cut out bread, butter, milk, sugar, beer and potatoes and to live on mainly animal protein, fruit and non-starchy vegetables. About nine months later, Banting had lost 35 pounds and his quality of life had significantly improved. He then self-published A Letter on Corpulence detailing his journey and gave copies away for free.
Banting’s ideas appealed to men with sedentary desk jobs, courtesy industrialisation, who feared that their bodies were becoming too soft and feminine, and weight loss became a way to reclaim their masculinity.
Women in the 1830s were perceived as emotional and lacking self-control, and therefore not built for the rigours of dieting. In this patriarchal society, beauty did not prioritise thinness and plumpness was associated with wealth, motherhood, and fertility.
The beauty standards around the female body slowly shifted in the 1890s when diet advice began appearing in American women’s magazines, and a scientific racism emerged to prove the superiority of the white race. Black women were characterised by their “presumed inability to control” their consumption, while white women were encouraged to diet, as a way to differentiate themselves from stereotypes of Black women.
By the 1920s, following World War I, social activities that were once supervised at home (such as the Bridgerton-type dating) became public. Western culture rapidly changed as knee-length skirts were replaced by shorter ones or trousers. People went out to the movies and jazz clubs, and the flapper appeared, so that women sported a thin, youthful body type with short hair, exposing skin and smoking in public. Thinness was hot, and plumpness was not.
As the demand for weight loss increased, people began to develop strategies to achieve this. Did you know that calorie counting originated as a food rationing technique during World War I? Dr Lulu Hunt Peters, an American physician, in 1918 popularised the concept of calorie counting for weight loss in her book, Diet & Health: With Key to the Calories. She believed that in wartime, it was criminal to hoard food in your anatomy. The fact is that Dr Peters’ work led to fat people being characterised as unpatriotic threats to the US, much as it sounds Trumpesque!
After World War II, food and advertising advanced and ideal standards of citizenship, femininity and the nuclear family developed.
This was perhaps the first time that amphetamines previously used by soldiers to combat stress were marketed to American women as diet pills. Later fad diets, like the grapefruit diet, cabbage soup diet, etc became popular.
One of the most famous diet programmes in the US, Weight Watchers began in 1962 and the term lifestyle change was introduced. During the 1960s in the US, a wave of social and political upheaval—from the Civil Rights Movement and Second Wave Feminism to anti–Vietnam War protests—challenged the status quo. Fat acceptance and fat liberation movements emerged, confronting the social, political, and economic systems that marginalise fat people and protesting discrimination.
Despite the growing fat acceptance movements, dieting pressures grew in the 1970s and 80s.
Exercise classes became increasingly popular for individuals hoping to slim down. American actress Jane Fonda’s at-home workout videos sold 17 million copies between 1982 and 1985, Lean Cuisine and Diet Coke offered low-fat, low-sugar, and low-calorie options.
In the 1990s and 2000s, the “waif” aesthetics, popularised by British model Kate Moss, encouraged an androgynous and emaciated body as the beauty ideal. As Paris Hilton and Britney Spears opened up conversations about the size of these women’s bodies, pressures to conform to a thin body type, awareness about eating disorders also increased.
As people began to feel pressured to diet and lose weight, the ideas of body positivity and body neutrality came to light. It was realised that anti-fatness as a system of oppression negatively impacts one’s physical, mental, and social well-being.
In our culture, food has played a central role in celebrations and festivities. Sweets are frequently distributed as gifts and eating out has become common for many occasions. “In some families, a heavier body weight—especially in children—is sometimes perceived as a sign of good health and prosperity, which can delay recognition of obesity as a health concern,” observes Dr Asma Ahmed, Consultant Endocrinology at The Aga Khan University Hospital. “This perception is not limited to the general public. Obesity is still not widely recognised as a chronic disease even among healthcare professionals in our country.”
“However, as these children reach adolescence and puberty, they frequently face bullying and social stigma,” she adds. “The stigma is particularly greater for women, who often feel pressured to meet certain body size expectations. Weight stigma is present in many parts of society—within healthcare systems, schools, workplaces, communities, and particularly in the media. Hurtful language and unsolicited advice can increase feelings of guilt and shame, preventing individuals from seeking appropriate medical care.”

The weight of shame
According to Dr Chooni Lal, Professor and Head of Department of Psychiatry and Behavioural Sciences at JPMC, Karachi, weight stigma can deeply affect how a person feels about themselves. “When someone is repeatedly judged, bullied or stereotyped because of their body size, it can slowly change the way they see their own worth,” he shares. “Over time, many people begin to feel embarrassed in their own bodies or start believing that their value as a person is somehow directly linked to their weight. That can slowly but surely erode away their confidence and self worth and leave someone feeling lonely, anxious, or emotionally exhausted. For some, it can also contribute to depression.
Dr Lal explained that it’s often overlooked that shame rarely motivates people to become healthier. “In fact, it often has the opposite effect. Feeling constantly judged can create stress and emotional pain rather than encouragement,” he says. “Some people may turn to food for comfort, while others avoid gyms, public spaces or even social situations because they’re worried about being stared at or criticised.”
Even going to the doctor and seeking help can feel stressful if someone expects their concerns to be dismissed as “just about weight”. People usually make healthier and more lasting changes when they feel safe, respected, and supported. “When someone feels understood rather than judged, it becomes much easier to engage with their health and take small, meaningful steps forward,” he adds.
For many people, body weight is closely tied to how they see themselves, emphasises Dr Lal. “When medication leads to rapid weight loss, it can bring relief, happiness, or a boost in confidence, especially for those who have struggled with their weight for years. At the same time, such a quick and visible change in the body can feel unfamiliar, and it may take time for someone to adjust to what they see in the mirror.”
He further explains, “People who have lived in a larger body for a long time often carry memories of being judged, excluded, or treated differently. Losing weight doesn’t automatically erase those experiences, and a person’s inner sense of self may not immediately match their new appearance. When others suddenly respond more positively after weight loss, it can also bring mixed feelings. Some people may feel pleased, while others may question why acceptance seemed to depend so much on body size.”
 Because of these emotional adjustments, rapid weight loss can sometimes feel psychologically complex as well as physically noticeable. “For this reason, it’s important that such treatments are approached with realistic expectations and, when needed, psychological support to help individuals process the changes and adjust to their new sense of self,” stresses Dr Lal.
Because of these emotional adjustments, rapid weight loss can sometimes feel psychologically complex as well as physically noticeable. “For this reason, it’s important that such treatments are approached with realistic expectations and, when needed, psychological support to help individuals process the changes and adjust to their new sense of self,” stresses Dr Lal.
Medications can make weight loss more achievable for many people, but they can also bring new kinds of pressure. “After losing weight, some individuals may feel an unspoken expectation from themselves or from others to maintain a certain body size,” he says. “That pressure to ‘stay that way’ can sometimes feel difficult to live up to. There can also be worry about what happens next. Some people feel anxious about regaining weight if they stop the medication, which can create stress or a sense of relying on the treatment to keep things stable. Rapid weight loss can also bring more attention from others' comments, compliments, or questions which doesn’t always feel comfortable and may make someone more aware of their body than before.”
Dr Lal maintains that while these medications can ease some of the challenges people face around weight, they don’t necessarily remove the social and emotional pressures tied to body image. “Over time, it helps to keep the focus on overall health, self-acceptance, and feeling comfortable in one’s own body, rather than feeling defined by a number on the scale,” he explains.
Repeated cycles of dieting and regaining weight, often called weight cycling, can take a real emotional toll over time. “Diets usually begin with hope and determination, but when the weight returns, people often feel disappointed or frustrated,” Dr Lal reveals. “Many start to blame themselves or feel as though they have failed, even though weight regain is a very common biological response. Over time, this pattern can slowly chip away at confidence and self-esteem.
It can also lead to an unhealthy relationship with food and body image. People may become overly focused on calories, body size, or the number on the scale, and eating can start to feel tied to guilt or strict rules rather than nourishment.
Because of this, there is growing recognition that the conversation needs to shift away from weight alone and toward overall wellbeing. Supporting sustainable habits such as balanced eating, enjoyable physical activity, good sleep, and looking after mental health tends to be far more helpful in the long run. When wellbeing is viewed more broadly, people are more likely to develop a kinder and more sustainable relationship with their bodies.”
 Then came a lizard
Then came a lizard
The story of the modern weight-loss revolution begins with an unlikely creature: the Gila monster. This venomous desert dweller’s saliva contains compounds that mimic GLP-1, a glucagon-like peptide hormone your intestines naturally produce. This discovery led to medications that represent the largest shift in weight management since the 1990s.
For decades, the weight-loss formula seemed simple: eat less, move more. Push harder. In 2022, when medicines came in, obesity was officially reclassified as a complex chronic disease.
Deep in the human brain, the hypothalamus controls appetite and fat storage. A disruption of this system creates a cruel feedback loop – the more weight you gain, the hungrier you feel, instead of being the other way round. This is what makes losing weight so difficult.
“Our body is smart and responds to weight loss by producing hormones such as ghrelin, which increases hunger, and lowers hormones like leptin, which normally help us feel full,” says Dr Ahmed. “This hormonal response increases hunger after weight loss and makes it challenging to maintain the reduced weight. The weight gain that often occurs after weight loss is due to this biological response. Understanding this can help individuals make changes that support keeping the weight off.”
This hormonal conspiracy against the body slows down our metabolism. Doctors have discovered astounding new connections between metabolism, addiction, behaviour, and chronic disease, and describe it as trying to climb out of a hole while someone keeps making it deeper.
“The relationship between weight loss, metabolism, addiction and chronic disease is increasingly recognised in medical and public health,” says Dr Ahmed. “These factors are interconnected through brain reward system, behaviour patterns and metabolic health. Our brain’s reward system along with environmental influences, is closely linked to the food choices we make and can contribute to addictive eating behaviors. Weight loss leads to substantial improvements in overall metabolic health, which can help improve chronic conditions such as diabetes, hypertension, high cholesterol, and fatty liver disease, cardiovascular disease, and sleep apnea.”
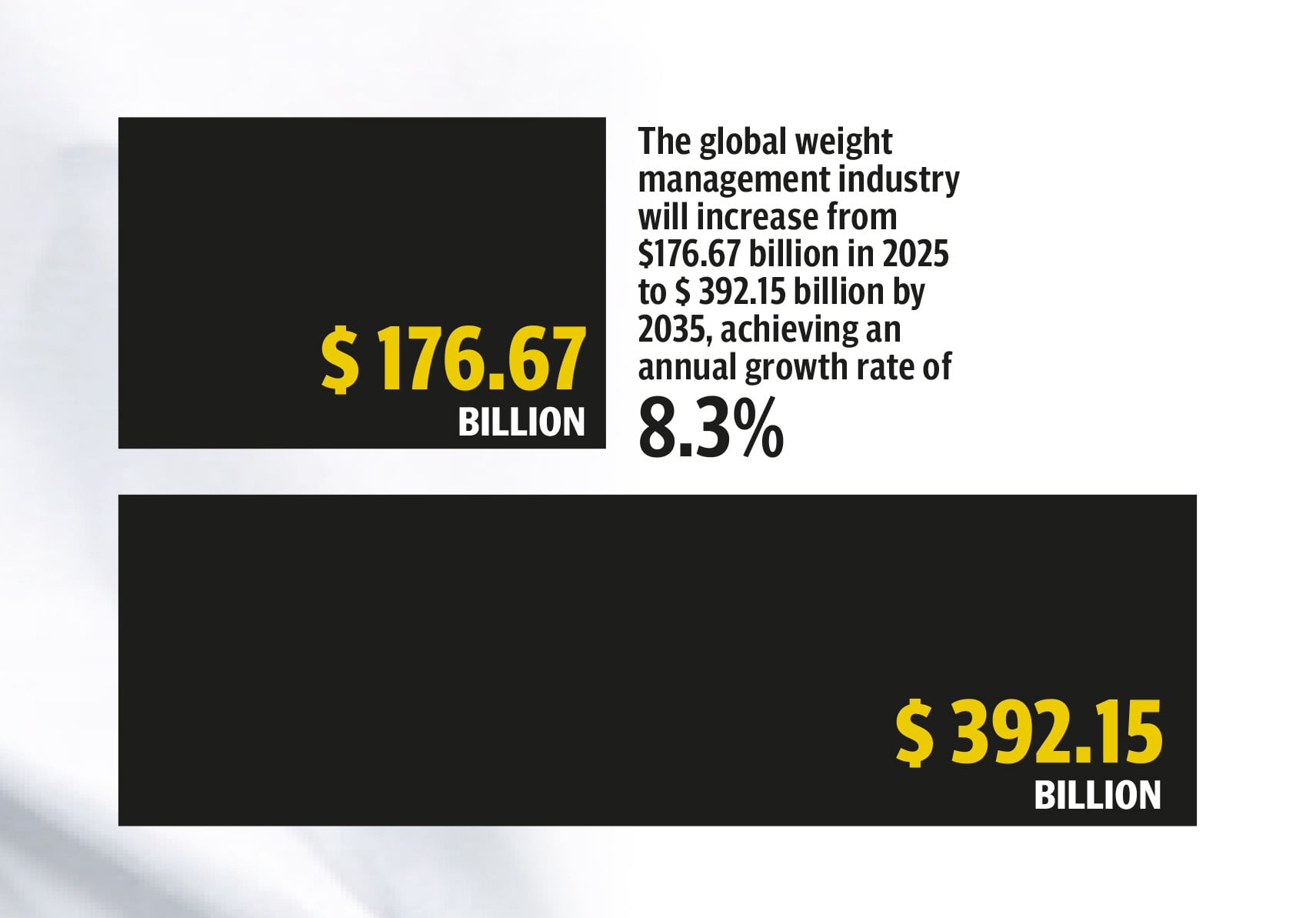
Statistics show that 2.5 billion people worldwide are overweight, with one billion classified as obese. That includes 350 million children. Now that obesity is considered a disease, meds are the logical solution.
 A plot twist
A plot twist
Medicines for diabetes reveal astounding metabolic and brain connections. The weight loss revolution, centred on GLP-1 agonists like Wegovy, Mounjaro, and Ozempic, is designed for individuals with obesity or overweight, particularly those struggling with related chronic conditions. These treatments aim to address the complex biological drivers of weight gain rather than relying solely on willpower. It is not about self-control, it is about the pill fixing it for you.
The quick fix
People with low body weight or those looking to lose only a few pounds for cosmetic reasons (as their wedding comes closer) are using these drugs.
Promoted and projected as “lifestyle enhancers", the soft image leads to increased demand, misuse and abuse, along with creating shortages for real patients who actually need them.
While everyone has seen photos of an emaciated-looking Demi Moore, a frail-looking Karan Johar and a starved Oprah Winfrey, has the Ozempic trend caught up with us locally?
“This trend has become increasingly common and has both advantages and disadvantages,” says Dr Ahmed. “The availability of these drugs in cosmetic clinics has also reinforced the perception that these treatments are for aesthetic purposes, which is a misconception.”
According to Dr Ahmed, the availability of these medications has improved significantly in recent years. “Both imported and locally produced biosimilar options are now available, and the choice often depends on affordability,” she notes. “The increased availability has also placed greater responsibility on physicians to ensure that these medications are prescribed to patients with appropriate indications.”
What happens when you stop GLP-1 meds
In a new review published in the journal eClinicalMedicine, 48 studies analysed and predicted the outcomes of people who either had diabetes or were overweight or obese and took popular GLP-1 medications. When they stopped taking GLP-1 weight-loss medications, they regained about 60% of the weight they lost within a year. Although doctors believe that some people will gain more weight than others as it varies with each individual.
Some people can come off of them and maintain the weight loss, others will need to wean off, while some may have to stay on the same dose of medicines forever.
Although GLP-1 medications have been successfully shown to help people lose some weight overall, doctors believe that it is best to adopt a healthy lifestyle, with exercise so as to avoid going back to GLP-1 meds or at least try to be dependent on them only in minimal doses.

Body image politics
The so-called “Ozempic era” inevitably collides with body image politics.
“The popularity of these medicines has intensified the ideal body image that equates thinness with beauty, success and self-discipline,” explains Dr Ahmed. “Moreover, rapid weight loss among celebrities and influencers has also created significant hype around these treatments. At the same time, social media videos and discussions about side effects have created fear and hesitation among people who may truly need these treatments. The best way to address this is to encourage individuals to seek advice from doctors with expertise in this area who can provide accurate information and answer their concerns.”
The drugs may be new, but the struggle between biology, beauty, and control is anything but.